Hospitals lack nurses and other health care workers despite the expansion of beds for COVID-19 patients, according to data from the OCTA Research Group.
In a webinar on April 23, Fr. Nicanor Austriaco, OP, a member of the research group, presented data that showed the gap between the number of nurses in hospitals and the bed capacity for COVID-infected patients.
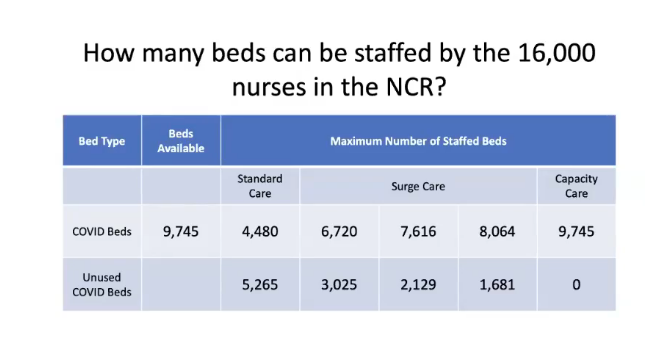
The report he presented titled “Spreadsheet Modeling of Nursing Staffing Capacity during a COVID-19 Surge” showed that the 16,000 nurses in the National Capital Region could not staff all the beds available for COVID-19 patients, citing data from the Department of Health.
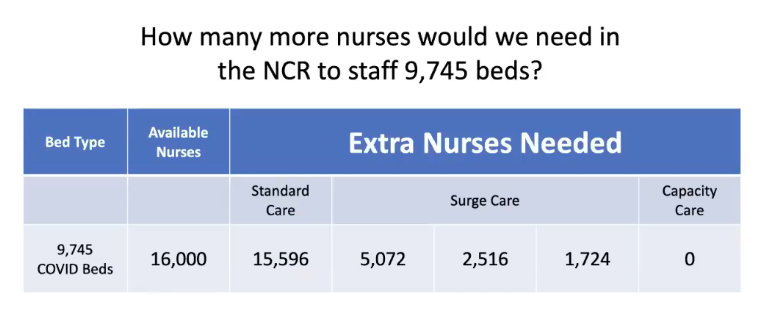
The research group’s data also showed that the region needed thousands more nurses to staff all the current 9,745 available beds in hospitals.
To achieve “full capacity care,” nurses have to staff twice the number of COVID-19 beds for “standard of care.”
Ratio needed:
- One nurse to eight COVID-19 ward beds
- One nurse to four COVID-19 intensive care unit beds
“We don’t have enough nurses to keep increasing the beds,” Austriaco said.
The priest-doctor also lamented how the government is only announcing more beds to “decongest” hospitals, but not hiring more health workers.
“One of the reasons why our hospitals appeared so overwhelmed in spite of extra number of beds recorded every single day in DOH data is because we are actually facing a log jam or limit. The limiting factor is actually not beds, but nurses,” Austriaco said.
He also pointed out that hospitals take too long to decongest because patients admitted there spend 27 days or nearly a month on average.
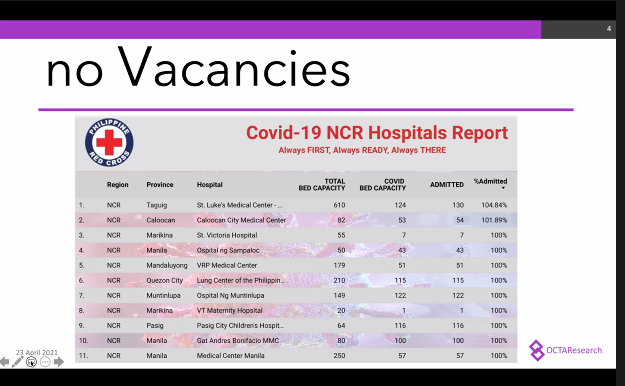
Similarly, another fellow Dr. Michael Tee presented data that all hospitals in the NCR have already reached hospital capacity as of April 22, citing data from the Philippine Red Cross operations center.
In the graph Tee showed, St. Luke’s Medical Center in Taguig and Caloocan City Medical Center are operating at more than 100% of their capacities.
This does not include COVID-19 patients who are queued at the emergency rooms and at home.
Since the spike in COVID-19 infections in the past weeks, social media was filled with tragic tales of COVID-19 patients who died outside hospital care as told by their relatives and friends.
Some Filipinos later encouraged others to self-isolate if their cases were classified as mild or asymptomatic to prevent further congestion of health care facilities.
They shared different guidelines on the health care equipment to purchase and tips to take care of an infected household member.
Taking care of health care workers
To help resolve this shortage, Dr. Ranjit Singh Rye, another OCTA research fellow, highly recommended the hiring of more health care workers in line with expansion of hospital care from the national to the local level.
Rye noted that improvement or expansion should always include both the health care workers and hospital capacity to help the country’s response for another public health crisis in the future.
“OCTA believes the most important element in your health care system are your health care workers,” he said.
“When you expand capacity it’s not just about beds and ventilators, it’s about making sure you have health care workers available to take care of patients,” he added.
Rye also emphasized the need to take care of health workers, especially the ones in local communities.
“We have to take care of our health care workers both at the national and the local level by increasing their numbers and providing them the proper remunerations, by protecting them when they get sick,” he said.