The following is a roundup of some of the latest scientific studies on the novel coronavirus and efforts to find treatments and vaccines for COVID-19, the illness caused by the virus.
Immune response may explain rare clots after AstraZeneca vaccine
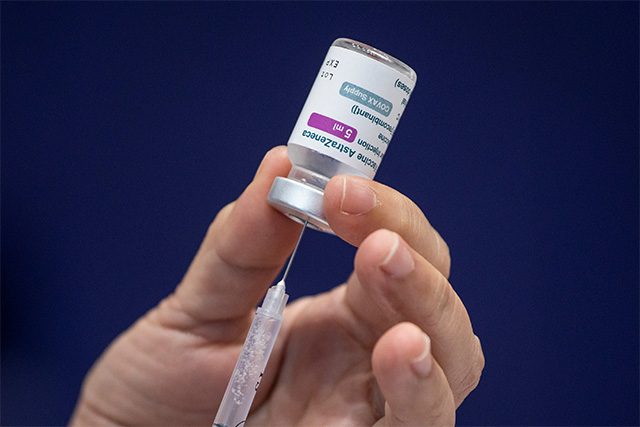
Researchers may have found an explanation for the rare but serious blood clots reported among some people who received AstraZeneca’s COVID-19 vaccine. They believe the phenomenon is similar to one that rarely occurs with a blood thinning drug called heparin, called heparin-induced thrombocytopenia (HIT).
In HIT, the drug triggers the immune system to produce antibodies that activate platelets, which cause blood to clot. Drugs other than heparin can cause clotting disorders that strongly resemble HIT, and researchers suspect that in rare cases, the AstraZeneca vaccine may be another such trigger.
Four previously healthy individuals who got the AstraZeneca shot and developed life-threatening clots had the same kind of antibodies that activate platelets and initiate clotting in HIT, the researchers reported on Monday in a paper posted on Research Square ahead of peer review.
Twenty individuals who received the vaccine but did not develop clots did not have these antibodies.
An editorial comment posted with the study noted that drug-induced thrombocytopenia is treatable if identified promptly.
Millions of people have received the vaccine without issues and European regulators and the World Health Organization say the benefits of the AstraZeneca shot outweigh its risks.
COVID-19 death risk rising for young adults in Brazil
Southern Brazil is seeing a sudden rise in COVID-19 deaths among young and middle-aged adults after the identification there of a concerning virus variant known as P.1, researchers said. They analyzed data from Parana – the largest state in southern Brazil – on 553,518 cases diagnosed from September 2020 through March 17, 2021.
In all age groups, the proportion of patients who died either held steady or declined between September and January. Starting in February, however, fatality rates rose for almost all groups over age 20, according to a report posted on Friday on medRxiv ahead of peer review.
From January to February, these rates tripled among patients aged 20 to 29, from 0.04% to 0.13%, and doubled among those aged 30 to 39, 40 to 49, and 50 to 59.
“Individuals between 20 and 29 years of age whose diagnosis was made in February 2021 had an over 3-fold higher risk of death compared to those diagnosed in January 2021,” the researchers said.
“Taken together, these preliminary findings suggest significant increases in case fatality rates in young and middle-aged adults after identification of a novel SARS-CoV-2 strain circulating in Brazil, and this should raise public health alarms.”
Pfizer, Moderna vaccines limit asymptomatic infections
Vaccines from Pfizer Inc and partner BioNTech SE and from Moderna Inc dramatically reduced the risk of infection by the new coronavirus within weeks after the first of two shots, according to data from a study of nearly 4,000 U.S. healthcare personnel and first responders in six states.
Previous trials by the companies evaluated the vaccines’ efficacy in preventing illness from COVID-19, but would have missed infections that did not cause symptoms.
In the new study, conducted from mid-December to mid-March, nearly 75% of participants had received at least one dose of vaccine, and everyone had weekly coronavirus testing for 13 consecutive weeks in order to pick up asymptomatic infections.
According to a report published on Monday by the U.S. Centers for Disease Control and Prevention (CDC), the risk of infection fell by 80% two weeks or more after the first of two shots and by 90% by two weeks after the second shot.
“The authorized mRNA COVID-19 vaccines provided early, substantial real-world protection against infection for our nation’s healthcare personnel, first responders, and other frontline essential workers,” CDC Director Rochelle Walensky said in a statement.
Pandemic has cut parents’ access to hospitalized children
Pediatricians have long endorsed the idea that babies and children in hospitals should not be separated from their families – a practice that in many facilities was restricted or discontinued to limit COVID-19 infections, according to new research.
From mid-May through early July, researchers collected survey responses from 96 pediatric care units in 22 countries in Europe, Asia, and North America.
The results – mostly from intensive care units for newborns – showed that before the pandemic, 87% of units welcomed families and 92% encouraged skin-to-skin care, according to a report published in Journal of Perinatology.
After the onset of the pandemic, more than 83% of the hospital units restricted family presence, with additional restrictions placed on parental participation in their infant’s care, said study coauthor Ita Litmanovitz of Meir Medical Center in Kfar Saba, Israel.
Hospitals’ decisions to limit family access did not depend on their previous rules, the availability of single-family rooms, or the virus infection rate in the hospital’s geographical area.
“Restrictions during the pandemic increased separation between the infant and family,” the researchers found.
These restrictions, Litmanovitz added, “go against psychological and neuroscientific evidence in support of unrestricted parental presence and ability to care for their hospitalized infants.”
—Reporting by Nancy Lapid; Editing by Bill Berkrot